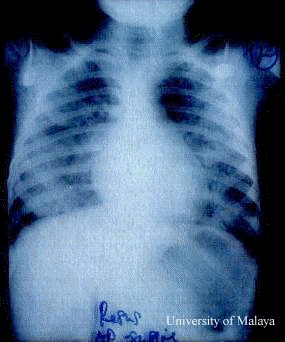
This article written by Dr. Lucy CS LUM helps explain the pulmonary edema seen in EV71 brainstem encephalitis.
Neurogenic pulmonary edema (NPE)
The association of pulmonary edema with CNS disease without underlying cardiopulmonary disease is known as neurogenic pulmonary edema (NPE). NPE is characterized clinically by an often fulminant course marked by pulmonary vascular congestion, protein rich edema fluid and intra-alveolar hemorrhage.
The association between CNS injury and pulmonary edema was first reported by Moutier in 1918; he observed the frequent occurrence of fatal acute pulmonary edema after cerebral trauma from war injuries. Since then NPE has been reported in a wide variety of CNS injuries such as raised intracranial pressure, brain tumour, seizures, intracerebral hemorrhage, subarachnoid hemorrhage, bulbar poliomyelitis, Guillain Barre and Reye’s syndromes. Several clinical and experimental observations point towards involvement of the medulla in the pathogenesis of NPE. To date, only 3 reports relate NPE in man to specific brainstem lesions :
Schlesinger. Neurogenic pulmonary edema due to puncture wound of the medulla oblongata; J Nerv Ment Dis 102: 247-255, 1945.
Baker AB. Poliomyelitis. A study of pulmonary edema. Neurology 7:743-751,1957.
Brown RH et al. Medulla oblongata edema associated with neurogenic pulmonary edema. J Neurosurgery 64:494-500, 1986.[MEDLINE abstract]
Baker’s description is particularly interesting because EV71 and polioviruses are enteroviruses. In his study of NPE following poliomyelitis, Baker noted that only patients with pathologic changes in the region of the dorsal nucleus of the vagus and the medial reticular nuclei of the medulla developed NPE. The pathogenesis of NPE is not so well defined but the physiologic changes have been described. Following an insult to the brainstem, there appears to be an overwhelming outpouring of catecholamines, esp noradrenalin. This produces peripheral vasoconstriction followed by systemic hypertension and a shift of blood from the high resistance systemic circulation to the relatively low resistance pulmonary circulation. This elevation in hydrostatic pressure damages the pulmonary capillaries with subsequent pulmonary hemorrhages. Experimental data also point towards an increase in pulmonary capillary permeability; thus the protein rich edema fluid. It is also shown in clinical studies that the heart suffers a severe knock : myocardial necrosis and echocardiographic evidence of severe cardiac dysfunction. It is the latter that might be misinterpreted as myocarditis. It has been argued that this may represent centrally mediated cardiac failure secondary to severe increase in left ventricular afterload.
References :
Mayer SA et al. Cardiac injury associated with neurogenic pulmonary edema following subarachnoid hemorrhage. Neurology 1994;44:815-820 [MEDLINE Abstract]
Sato K et al. Left ventricular asynergy and myocaridal necrosis accompanied by subarachnoid hemorrhage.J. Cardiology 1990: 20:2, 359-367.[MEDINE Abstarct]
- Lucy CS LUM, MBBS, MRCP.
- Lecturer, Department of Pediatrics,
- University Malaya Medical Center,
- 50603 Kuala Lumpur.
- e-mail : pattans@pc.jaring.my
Search MEDLINE Neurogenic Pulmonary Edema [MEDLINE Abstracts]
Back to Enterovirus Outbreak site
Back to Vads Corner
11 July 1998